Case Insight: Diabetic Foot Ulcer and Wound Management
Introduction
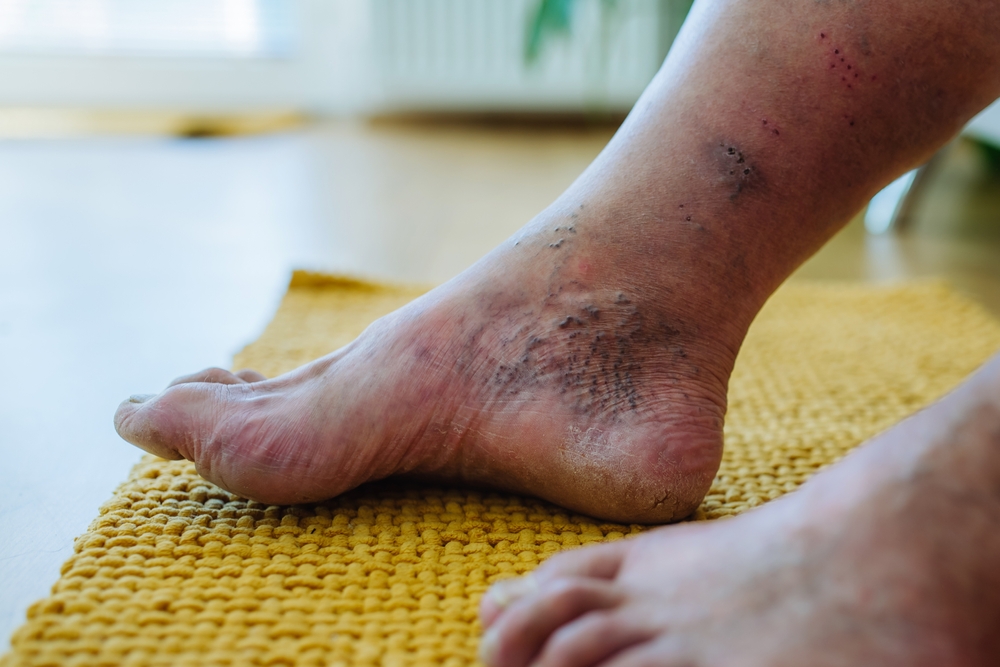
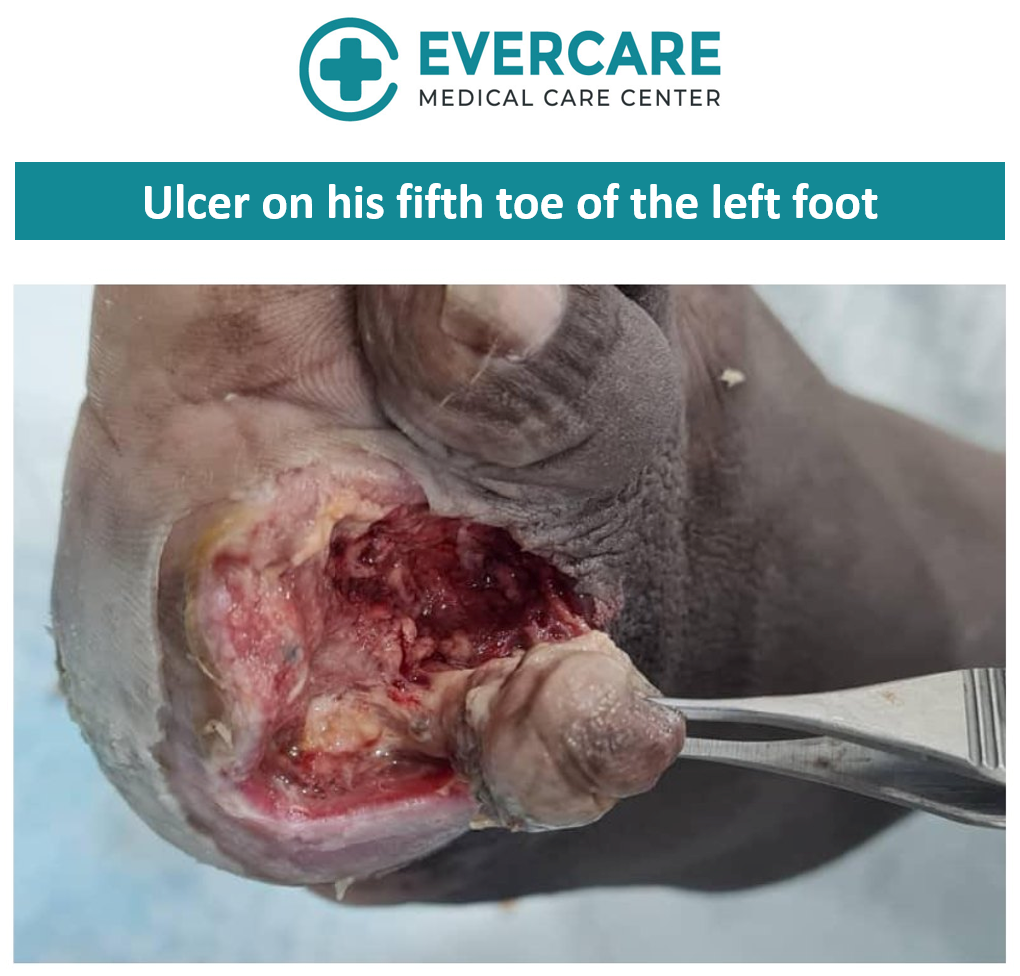
We would like to share a clinical case (published with patient consent) involving one of our patients, a 66-year-old individual who presented with a diabetic foot ulcer affecting the fifth toe of the left foot. The patient also had underlying conditions including diabetes mellitus, hypertension, and dyslipidaemia.
Diabetic foot ulcers are a common but potentially serious complication, particularly in patients with multiple medical conditions. Early recognition and appropriate management are important to prevent progression and complications.
Understanding Diabetic Foot Ulcers
Diabetic foot ulcers often arise due to a combination of factors, including reduced blood circulation, nerve impairment (neuropathy), and prolonged pressure on specific areas of the foot.
Reduced sensation may cause patients to be unaware of minor injuries, allowing wounds to develop and worsen over time. In addition, underlying conditions such as diabetes and vascular issues may further delay the healing process.
Effective management requires a comprehensive approach in a proper setting that addresses both the wound and the contributing systemic factors.
Treatment Approach
Management of diabetic foot ulcers involves a structured and coordinated care plan under clinical supervision.
This typically includes:
- Appropriate wound cleansing and dressing
- Offloading pressure from the affected area
- Monitoring for signs of infection
- Regular follow-up to assess healing progress
In this case, a treatment plan was implemented incorporating wound care and offloading measures, with close monitoring throughout the treatment period.
While the underlying causes differ, similar principles of structured wound care and ongoing monitoring apply across conditions, as seen in this chronic venous ulcer case, where targeted management supports healing.
Healing Progress
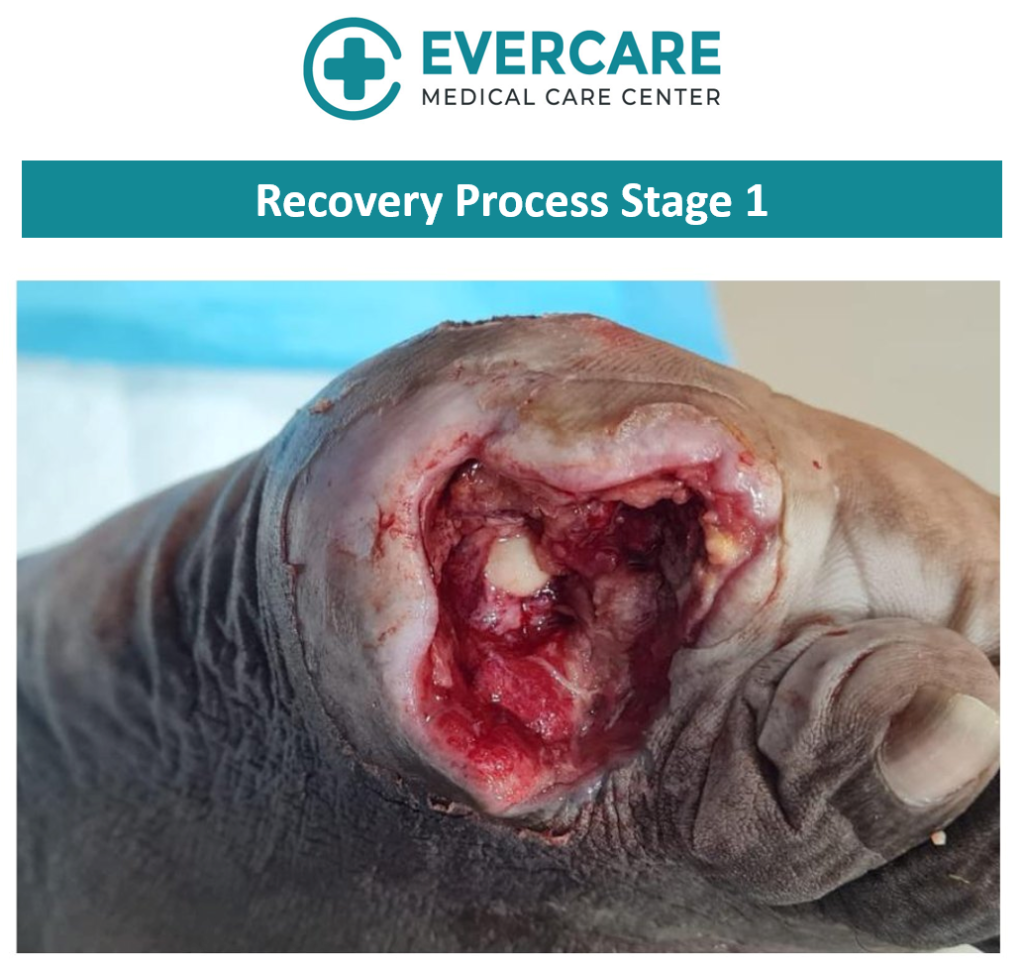
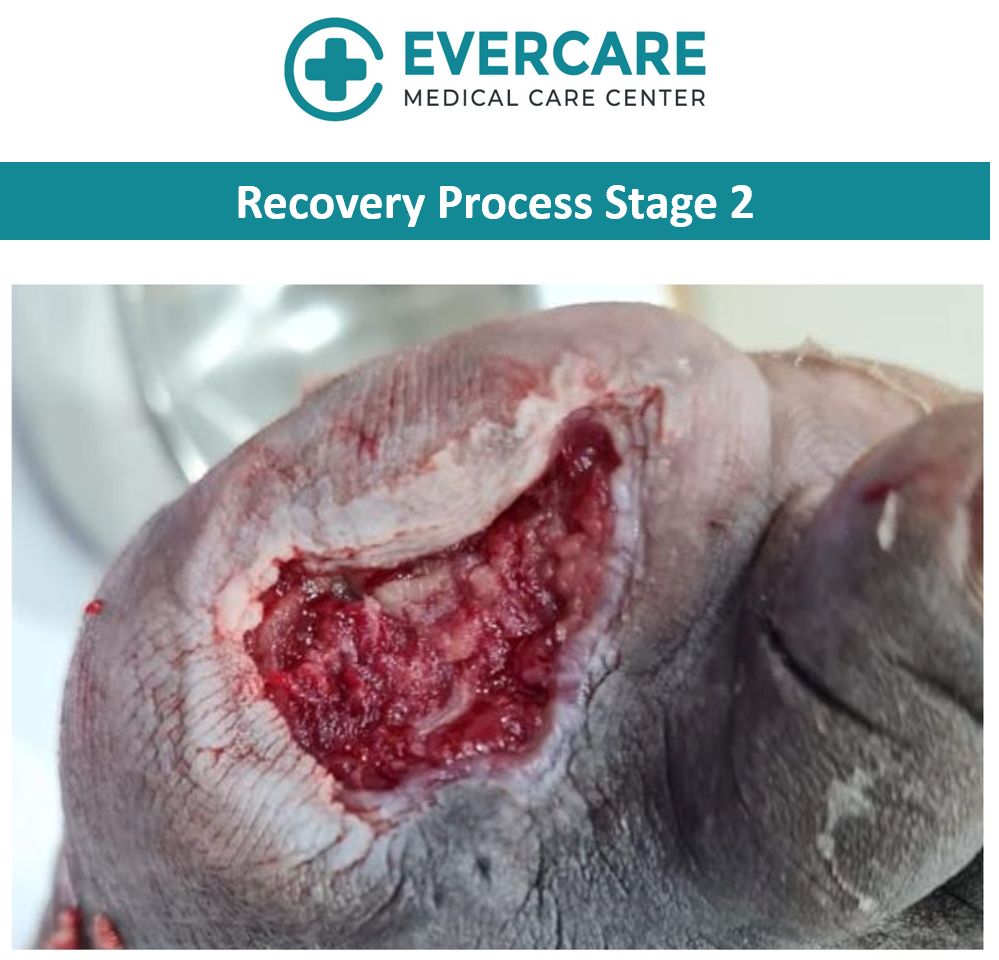
With consistent care and adherence to treatment recommendations, gradual improvement in the wound condition was observed over time.
Healing timelines may vary depending on the severity of the wound, underlying health conditions, and how early treatment is initiated. Regular monitoring allows for timely adjustments to the care plan to support optimal healing.
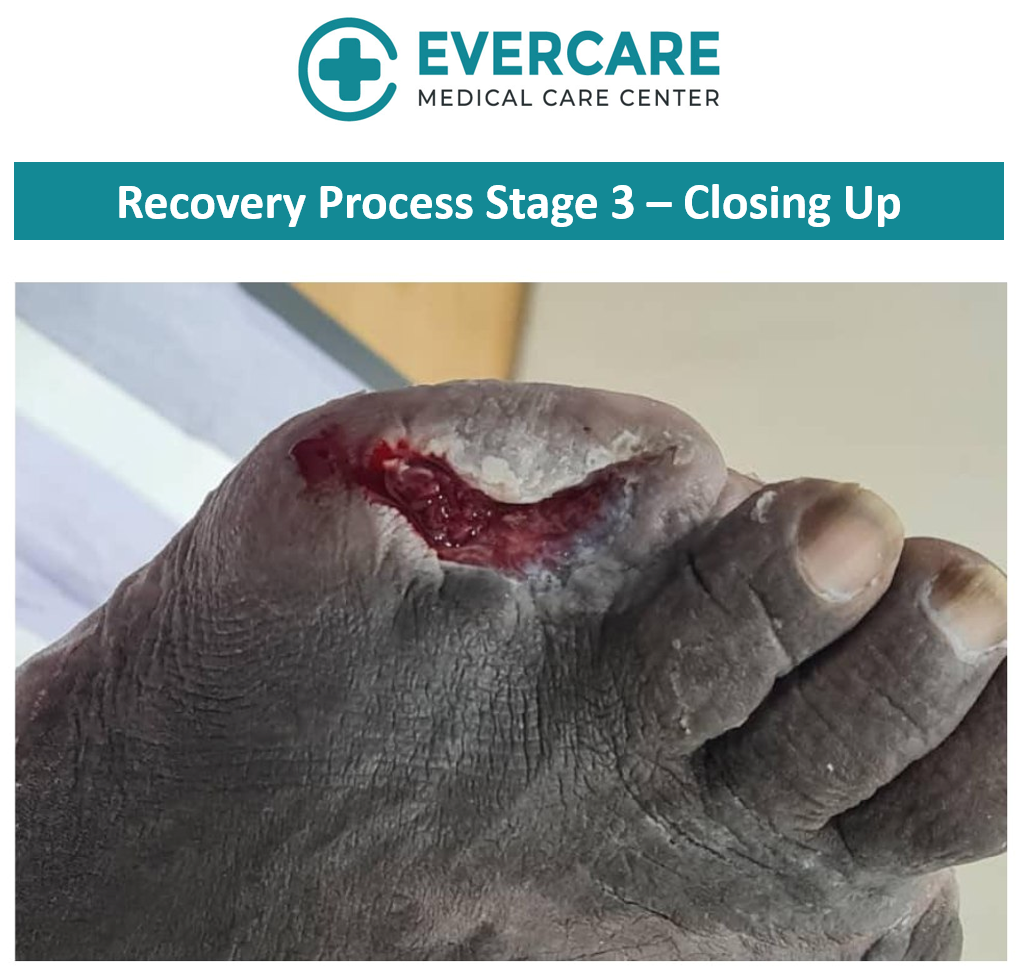
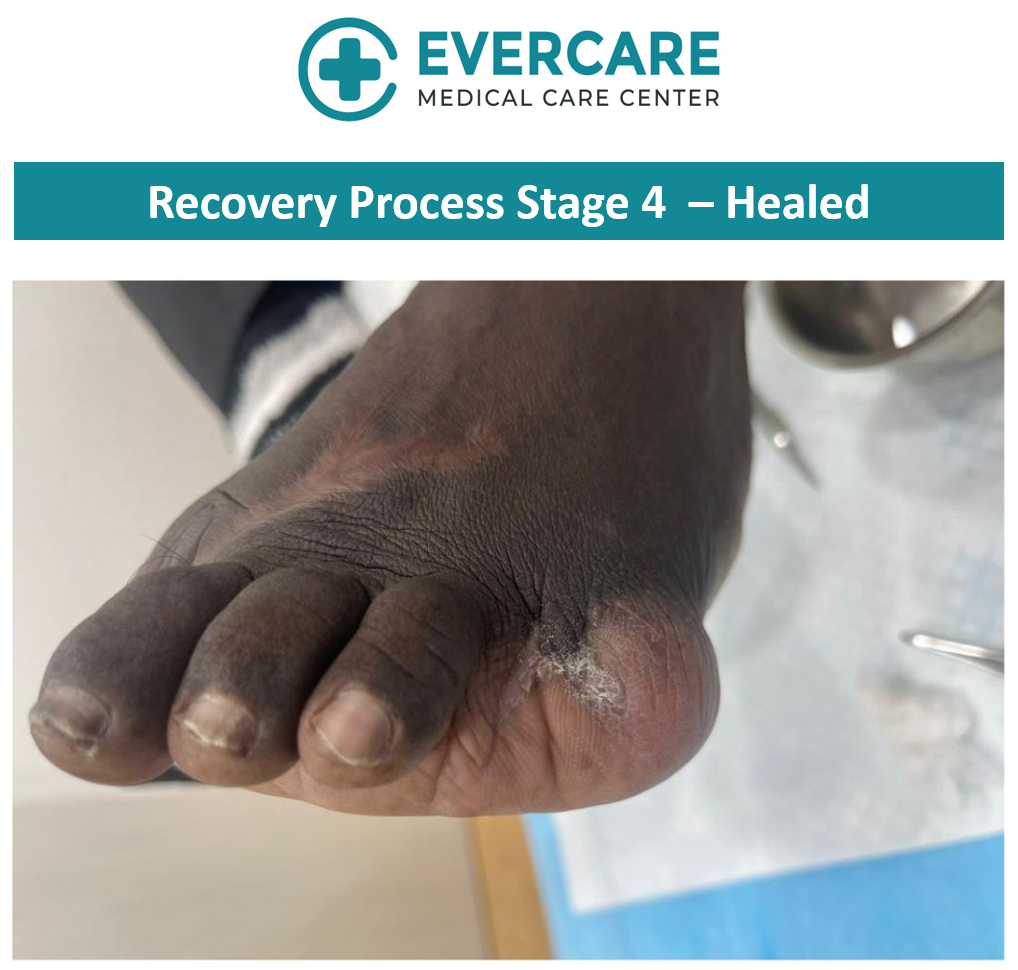
Key Insights
Diabetic foot ulcers require early recognition and a structured approach to management. Delayed treatment may increase the risk of complications, including infection and prolonged healing.
Consistent wound care, effective pressure offloading, and management of underlying conditions play a key role in supporting healing and reducing complications in diabetic foot ulcers.
– Dr Sreedharan Muniandy
Advanced Wound Care Centre
Evercare Medical Care Centre, Penang, Malaysia.
Disclaimer
Images are shared with patient consent for educational purposes. Individual outcomes may vary depending on overall health and adherence to treatment.
